Medical Myths: All about stroke
According to the Centers for Disease Control and Prevention (CDC)Trusted Source, over 795,000 people in the United States have a stroke every year, and around 610,000 are first strokes.
In 2019, stroke was the leading cause of mortality globally, accounting for 11% of deaths.
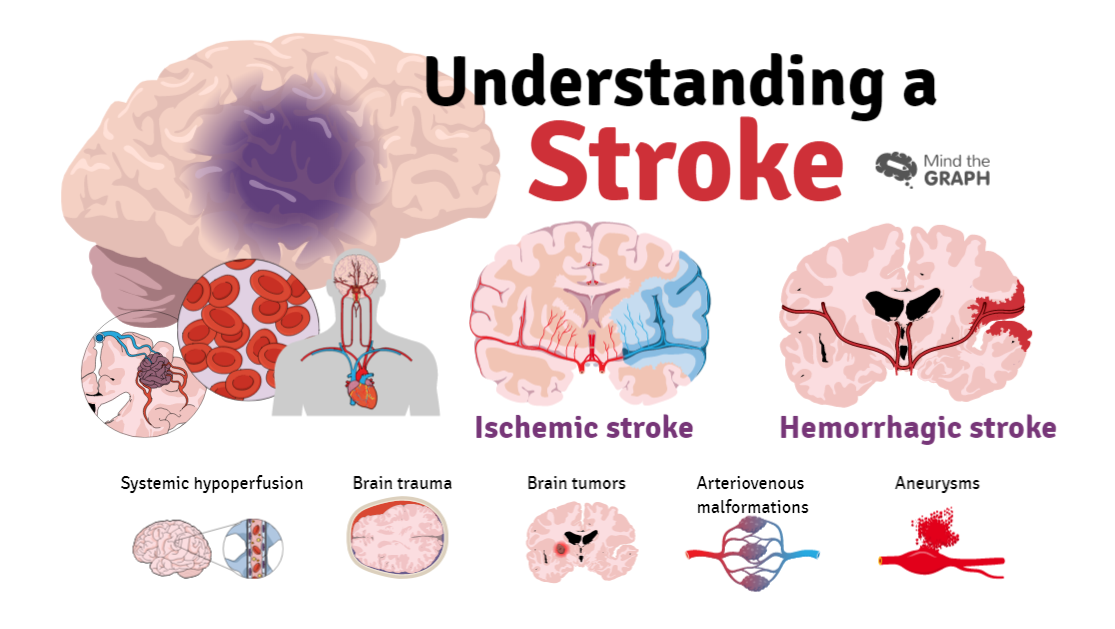
There are three main types of stroke. The first and most common, accounting for 87% of cases, is an ischemic stroke. It occurs when blood flow through the artery that supplies oxygen to the brain becomes blocked.
The second is a hemorrhagic stroke, caused by a rupture in an artery in the brain, which in turn damages surrounding tissues.
The third type of stroke is a transient ischemic attack (TIA, which is sometimes called a “ministroke.” It happens when blood flow is temporarily blocked to the brain, usually for no more than 5 minutes.
While stroke is very common, it is often misunderstood. To help us dispel myths on the topic and improve our understanding, we got in touch with Dr. Rafael Alexander Ortiz, chief of Neuro-Endovascular Surgery and Interventional Neuro-Radiology at Lenox Hill Hospital.
1. Stroke is a problem of the heart
Although stroke risk is linked to cardiovascular risk factors, strokes happen in the brain, not the heart.
“Some people think that stroke is a problem of the heart,” Dr. Ortiz told MNT. “That is incorrect. A stroke is a problem of the brain, caused by the blockage or rupture of arteries or veins in the brain, and not the heart.”
Some people confuse stroke with a heart attack, which is caused by a blockage in blood flow to the heart, and not the brain.
2. Stroke is not preventable
“The most common risk factors [for stroke] include hypertension, smoking, high cholesterol, obesity, diabetes, trauma to the head or neck, and cardiac arrhythmias,” said Dr. Ortiz.
Many of these risk factors can be modified by lifestyle. Exercising regularly and eating a healthy diet can reduce risk factors such as hypertension, high cholesterol, obesity, and diabetes.
Other risk factors include alcohol consumption and stress. Working to reduce or remove these lifestyle factors may also reduce a person’s risk of stroke.
3. Stroke does not run in families
Single-gene disorders such as sickle cell disease increase a person’s risk for stroke.
Genetic factors including a higher risk for high blood pressure and other cardiovascular risk factors may also indirectly increase stroke risk.
As families are likely to share environments and lifestyles, unhealthy lifestyle factors are likely to increase stroke risk among family members, especially when coupled with genetic risk factors.
4. Stroke symptoms are hard to recognize
The most common symptoms for stroke form the acronym “F.A.S.T.“:
- F: face dropping, when one side of the face becomes numb and produces an uneven “smile”
- A: arm weakness, when one arm becomes weak or numb and, when raised, drifts slowly downward
- S: speech difficulty, or slurred speech
- T: time to call 911
Other symptoms of stroke include:
- numbness or weakness in the face, arm, leg, or one side of the body
- confusion and trouble speaking or understanding speech
- difficulty seeing in one or both eyes
- difficulty walking, including dizziness, loss of balance and coordination
- severe headaches without a known cause
5. Stroke cannot be treated
“There is an incorrect belief that strokes are irreversible and can’t be treated,” explained Dr. Ortiz.
“Emergency treatment of a stroke with injection of a clot busting drug, minimally invasive mechanical thrombectomy for clot removal, or surgery can reverse the symptoms of a stroke in many patients, especially if they arrive to the hospital early enough for the therapy (within minutes or hours since the onset of the symptoms),” he noted.
“The longer the symptoms last, the lower the likelihood of a good outcome. Therefore, it is critical that at the onset of stroke symptoms — ie. trouble speaking, double vision, paralysis or numbness, etc — an ambulance should be called (911) for transport to the nearest hospital,” he continued.
Research also shows that those who arrive within 3 hours of first experiencing symptoms typically have less disability 3 months afterward than those who arrived later.
6. Stroke occurs only in the elderly
Age is a significant risk factor for stroke. Stroke risk doubles every 10 years after age 55. However, strokes can occur at any age.
One study examining healthcare data found that 34% of stroke hospitalizations in 2009 were under age 65.
A review in 2013 points out that “approximately 15% of all ischemic strokes occur in young adults and adolescents.”
The researchers noted that stroke risk factors including hypertension, diabetes, obesity, lipid disorders, and tobacco use were among the most common co-existing conditions among this age group.
7. All strokes have symptoms
Not all strokes have symptoms, and some research suggests that symptom-free strokes are far more common than those with symptoms.
One study found that out of the over 11 million strokes in 1998, 770,000 presented symptoms, whereas close to 11 million were silent.
Evidence of these so-called silent strokes appears on MRI scans as white spots from scarred tissue following a blockage or ruptured blood vessel.
Often, silent strokes are identified when patients receive MRI scans for symptoms including headaches, cognitive issues, and dizziness.
Although they occur without symptoms, they should be treated similarly to strokes with symptoms. Silent strokes put people at risk of future symptomatic strokes, cognitive decline, and dementia.
8. A ministroke is not so risky
“The term ministroke has been used incorrectly as some think that it is related to small strokes that carry low risk,” said Dr. Ortiz. “That statement is incorrect, as a ministroke is a transient ischemic attack (TIA).”
“It is not a small stroke, but a premonition that a large stroke can occur. Any symptom of acute stroke, transient or persistent, needs emergency workup and management to prevent a devastating large stroke,” he added.
9. Stroke always causes paralysis
Stroke is a leading cause of long-term disability, but not everyone who has a stroke will experience paralysis or weakness. Research shows that stroke leads to reduced mobility in over half of stroke survivors aged 65 and over.
However, the long-term impacts of stroke vary on many factors, such as the amount of brain tissue affected and the area affected. Damage to the left brain, for example, will affect the right side of the body and vice versa.
If the stroke occurs in the left side of the brain, effects may include:
- paralysis on the right side of the body
- speech and language problems
- slow and cautious behavior
- memory loss.
If it affects the right side of the brain, paralysis may also occur, this time on the left side of the body. Other effects may include:
- vision problems
- quick and inquisitive behavior
- memory loss.
10. Stroke recovery happens fast
Recovery from stroke can take months, if not years. However, many may not fully recover. The American Stroke Association says that among stroke survivors:
- 10% will make an almost complete recovery
- another 10% will require care in a nursing home or another long-term facility
- 25% will recover with minor impairments
- 40% will experience moderate to severe impairments
Research suggests there is a critical time window between 2–3 months after stroke onset, during which intensive motor rehabilitation is more likely to lead to recovery. Some may also be able to spontaneously recover during this period.
Beyond this window, and beyond the 6-month mark, improvements are still possible although are likely to be significantly slower.
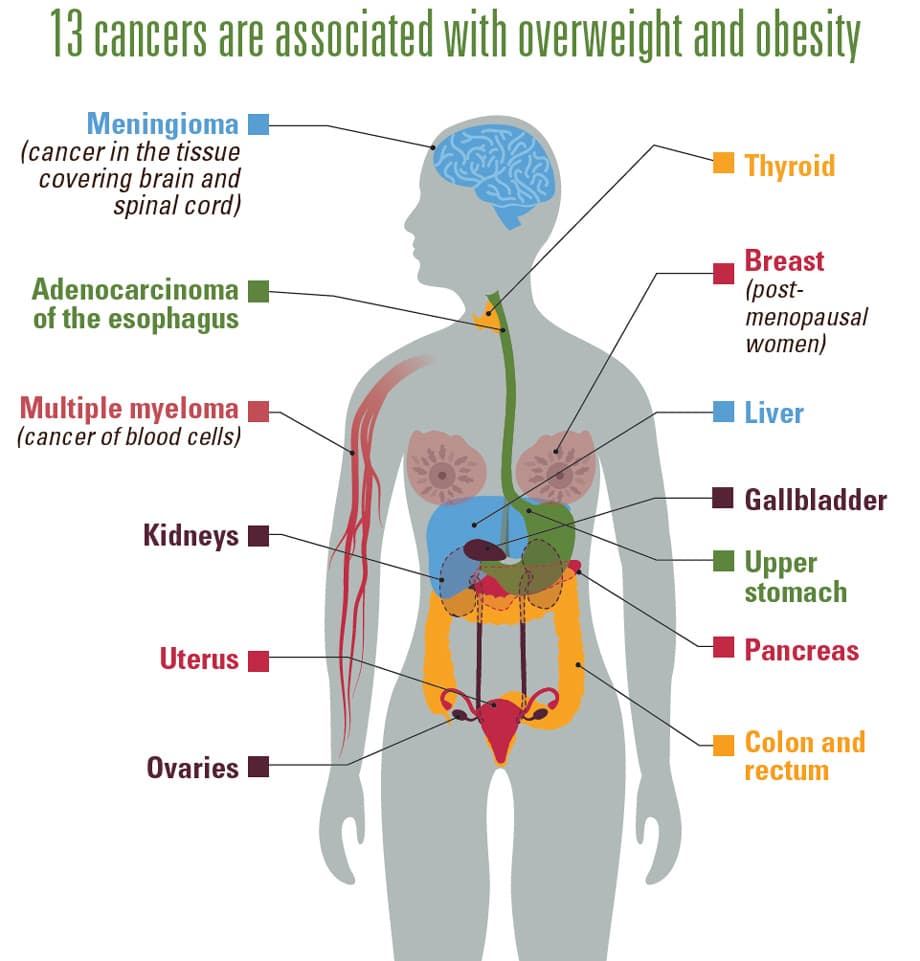
Cancer
Cancer
Cancer is one of our nation’s most feared diseases, with more than 1.6 million new cases diagnosed each year. But thanks to National Institute of Health (NIH) research, this number is now falling. Between 1991 and 2014, #cancer death rates went down 25 percent.
NIH research has transformed the way we think about cancer from affecting specific parts of the #body to a much more precise understanding of the molecular cause. For example, the drug pembrolizumab is one of a new class of cancer drugs that works by engaging a patient’s immune system to attack his or her tumors. Doctors already use this drug to treat some patients with several specific cancer types, including lung cancer and head and neck cancer. And, very recently, it became the first cancer therapy approved by the Food and Drug Administration (FDA) to treat any type of tumor, regardless of its location in the body, as long as the tumor has specific genetic features that make it much more likely to shrink after treatment with the drug. This is just one example of how genomics has revolutionized our understanding of cancer (see Precision Oncology, p.18).
Despite gains, there is much work to do. Many clinical trials are testing new targeted treatments, as well as combinations of different cancer therapies. With other federal agencies, NIH is participating in the Cancer MoonshotSM, a bold initiative to accelerate cancer research that aims to make more therapies available to more patients while also improving our ability to prevent cancer and detect it at an early stage.
Good Health for All
Many people in America are more likely to get certain #diseases and to die from them, compared to the general population. One of NIH’s greatest challenges is to understand and eliminate profound disparities in health outcomes for these individuals. We know the causes of health disparities are many. They include biological factors that affect disease risk; but most of the causes turn out to be non-biological factors such as socioeconomics, culture, and environment. Teasing apart health outcomes that differ among racial/ethnic groups is providing clues. For example, NIH research shows that among cigarette smokers, African Americans and Native Hawaiians are more susceptible to lung cancer than Whites, Japanese Americans, and Hispanics. Scientists are also intrigued by the “Hispanic paradox,” in which U.S. Hispanics often experience similar or better health outcomes across a range of diseases compared with non-Hispanic Whites. Understanding this advantage may help us identify contributing factors and effective interventions.
5 Public Health Crises Facing America
Public Health Crises: Five Big Ones Facing America Right Now
- Obesity
- Heart Disease
- Addiction/Substance Abuse
- Dementia
- Food Safety
Obesity, dementia, and heart disease – these are among some of the most concerning public health crises faced by the US today. Why are we facing some of these issues, and what are the known facts at this point? Follow along for the scoop on five of today’s most pressing public health crises in the US.
1. Obesity
The advantages of living in a modernized society include more luxury and more ready access to consumables of all sorts. This becomes a problem when the end result is obesity in a significant portion of the population. According to most research, the 1980s marked the beginning of the obesity epidemic in America today.
So, what does this particular health crisis look like? U.S. News shares that around 40 percent of Americans over the age of 20 are said to be obese. These numbers and the numbers of obese children are steadily on the rise. At the end of the day, what makes this such a critical issue overall is the fact that obesity is directly linked to early death and the onset and even further complication of diabetes, heart disease, liver disease, cancer, and many other ailments.
2. Heart Disease
As discussed above, heart disease itself is often a derivative of obesity. In other cases, it can be brought on by unhealthy lifestyle choices, environmental factors, and sometimes, genetics. At the end of the day, this condition is a major problem plaguing Americans’ health at present.
Heart disease, often called by several other names, is essentially stress and damage taken on by the heart that can worsen and lead to heart attacks, strokes, and even fatal events, ultimately in some cases. Factors that help to remediate the various forms of heart disease include healthy dietary choices, regular exercise, and avoidance of illicit drug and alcohol use. These remediating factors are many of those very same ones that Americans struggle to healthily maintain so often in today’s times.
3. Addiction/Substance Abuse
Addiction and substance abuse represent some of the most notable public health crises happening right now in the US. The reasons for this current epidemic are many and complex, but the effects of it are crippling to the individual sufferer and entire communities alike. According to the National Institute on Drug Abuse, an average of more than 130 people die each day in the US from opioid overdose alone. The economic burden placed on the country as a whole, just from prescription opioid abuse itself, is estimated by officials to be around $78.5 billion each year. With these kinds of figures, it’s easy to begin to see how detrimental this particular crisis has become in recent times.
4. Dementia
Dementia, the detrimental mental degradation associated with many cognitive diseases, is yet another looming and major public health crisis faced by the US right now. According to a group of top U.S. Surgeons General in a pivotal op-ed featured in the Orlando Sentinel recently, the public was made aware of the impending weight of the crisis at hand. It was therein estimated by experts that dementia numbers in the public double every five years and the numbers of those affected are unequivocally unprecedented and a potentially system-overwhelming problem.
5. Food Safety
Food safety is rated by a number of government and research organizations as another, top crisis concern for the US right now. This is because of the mass number of food producers, production associations, and even weak points in the continuum of the food markets. Food-born illness spread en-mass can quickly affect thousands of people, while cases of intentional endangerment to the food supply, such as through tampering or deceitful production practices, also can have major implications. For these many, compounding reasons, food safety in the US is a major concern today.
Public health crises can certainly be a great cause for concern. However, with the application of science and subsequent public awareness, many “worst-case scenarios” can be avoided altogether. As of now, the five above-mentioned public health crises are widely regarded as being among the most important and foreshadowing to address.
Men’s Mental Health: Warning Signs & Where to Go for Help
Men typically don’t want to discuss mental health issues, much less get treatment for one.
That’s a problem, given how many males struggle with mental health problems: Six million American men suffer from depression every year, while 3 million struggle with anxiety disorder, according to Mental Health America. Beyond that, 90% of those diagnosed with schizophrenia by age 30 are men, and 25% of those with binge eating disorder are males. Unfortunately, men are less likely to seek professional help for their problems.
When it comes to suicide, the picture is also troubling. While women are more likely to attempt suicide, it is the 7th leading cause of death among males, and white men over the age of 85 are the most likely to die by suicide.
Here, experts describe the most common mental health conditions men experience, the symptoms that may differ in men versus women, and what resources are available for those seeking help and treatment options.
Common mental health conditions in men
According to Mental Health America, the most common men’s mental health conditions are:
- Depression
- Suicide
- Anxiety
- Bipolar disorder
- Eating disorders
- Schizophrenia
- Substance abuse
“It’s a sign of strength to talk about these issues with your health care provider, counselor or a supportive family member or friend,” Piedmont Healthcare family medicine physician Dr. Siraj Abdullah said in a recent article. “As men, we tend to let stress build up until it affects our mental and physical health. Talking about your mental health is a way to take care of your body.”
How men’s mental health symptoms may show up differently than in women
The reasons that mental health symptoms can be different for men and women are complex, according to McLean Hospital chief of psychology Kathryn McHugh.
She noted in a hospital article that “biology is not the only piece of the puzzle. There are also many social and cultural factors that play a role in mental health and wellness, such as social role expectations, discrimination and violence.”
The Anxiety and Depression Association of America states that the main mental health symptoms in men that may be different from those found in women are:
- Abuse or misuse of drugs or alcohol
- Noticeable changes in mood, appetite or energy levels
- Violent, controlling or abusive behavior
- Digestive issues, headaches and pain
- Escaping into work, sports or other distracting behavior
- Risk-taking
Men with depression are also more likely than women to report symptoms of fatigue and loss of interest in work or hobbies, according to Mental Health America.
Men are particularly susceptible to suicide. According to the U.S. Centers for Disease Control and Prevention, men are four times more likely to die by suicide than women, and gay and bisexual men under the age of 25 are at a higher risk for attempting suicide than the general male population, according to Mental Health America.
The Suicide Prevention Resource Center notes that one of the reasons for higher male suicide rates is that men are less likely to get mental health care than women. The center suggests getting help before a mental health crisis occurs. This can include:
- Seeking behavioral health care, such as seeing a therapist
- Connecting to family, friends, community and social organizations
- Learning life skills like problem-solving and strategies for adapting to change
- Engaging with spiritual, religious or other belief practices that discourage suicide
If you’d like to begin or continue a behavioral health care plan, you can reach out to the SAMHSA National Helpline for a treatment referral.
Men’s mental health resources: How to get help
APA Psychologist Locator Tool
The American Psychological Association offers a database of thousands of therapists. Just put in your ZIP code, provider name or practice area. Once the results show up, you can sort the psychologists by a variety of categories, such as gender and treatment methods.
If you’re looking for a men’s mental health hotline to discuss your issues confidentially at no charge, the Mental Health Hotline provides a toll-free number with counselors on stand-by 24/7. The organization also lists several condition-specific hotlines for health issues like anxiety, depression, PTSD (post-traumatic stress disorder) and more — plus links to helpful resources on these conditions.
Fictional Dr. Rich Mahogany “runs” this site, which is actually administered by multiple agencies, including the Colorado Department of Public Health. It combines helpful mental health techniques and quizzes with humor and a uniquely human touch. There’s an online peer chat, 20-point head inspection and a worried-about-someone page to help loved ones of men who may be experiencing mental health issues.
Multicultural care meets mutual aid at Therapy for Black Men, where the coaches and counselors strive to offer free or discounted services to Black men with mental health issues. You can meet in person or online for a session, and there’s also a host of articles and social resources, including community organizations aimed at helping your mental health thrive.
Mental health medications
Several medications may be prescribed by your doctor to help you improve your mental health. According to the U.S. National Institute of Mental Health, these include:
- Antidepressants
- Anti-anxiety medications
- Antipsychotics
- Stimulants
- Mood stabilizers
If you’re experiencing a mental health crisis or suicidal ideation and need to talk to someone, call 988, the Suicide & Crisis Lifeline. The Lifeline offers free, confidential emotional support across the United States, 24 hours a day, 7 days a week.
US Mayors Cite ‘Unprecedented’ Mental Health Crisis as Top Concern
Substance abuse, homelessness and access to health services are among the issues that city officials say demand more resources in a new US Conference of Mayors survey.
An “unprecedented” mental health crisis is overwhelming US cities, which lack adequate resources to address growing challenges, according to a new report released today by the US Conference of Mayors. In recent years, the Covid-19 pandemic exacerbated mental health issues, particularly involving substance abuse, said a survey of mayors of 117 cities in 39 states.
“Addressing this surging mental health crisis is one of the most pressing issues facing America’s cities,” said Tom Cochran, executive director of the US Conference of Mayors, a nonpartisan organization of cities with populations of 30,000 or more. The report also cited “staggering increases in stress, depression, isolation, loneliness, and accompanying mental health hurdles faced by Americans of all ages.”
In a survey conducted this spring, 97% of mayors said requests for mental health services increased in their city in the past two years, but 88% lack resources to address the crisis. Participating cities spanned the US, and included Chicago; Seattle; Montgomery, Alabama; and Atlanta.
Substance abuse was the main cause for increasing mental health problems, 85% of cities reported. That was followed by Covid-19, homelessness and economic concerns.
Substance use disorders topped the list of mental and behavioral health problems in 65% of cities, followed by homelessness stemming from mental illness in 56%. Other challenges included shortages of mental and behavioral health workers, including school counselors, as well as a lack of access to behavioral health services.
Among youth, depression is the leading primary mental health problem, according to 89% of cities. More than 43% said teen suicide is a significant problem.
Nineteen cities called for more funding for services, but several noted that most funding goes to county — not city — governments.
Although the vast majority of cities reported inadequate mental health resources, 82% have developed new initiatives and/or increased funding to mental health programs. Ninety-three percent reported they have improved their emergency response to behavioral health crises. Meanwhile, 94% of cities said their police department provides mental health programs to officers.
Examples of initiatives cited in the survey include Mesa, Arizona, where its police department is coordinating with a nonprofit crisis line and system. Since 2018, the city has increased the types of emergency calls transferred, including children with behavioral issues, second-hand suicide reports, as well as dementia, psychosis, anxiety, PTSD, and basic problem-solving help. In 2022 alone, more than 3,500 911 calls were sent directly to its crisis hotline, away from Mesa’s police and fire departments, according to the city’s survey response.
In Las Vegas, an outreach team provides services to unhoused people to divert them from emergency rooms and into appropriate treatment. A crisis response team also works with the fire department to deescalate non-emergency mental health issues.
Long Beach, California, has established mobile homeless and behavioral health services, and teams of mental health clinicians to do homeless outreach. In 2022, Hartford, Connecticut, launched a non-law enforcement crisis intervention program in response to emergency 911 calls for people in mental health crises.
City leaders from Orlando, Florida, expressed their support for the “Housing First” model as a means of addressing homelessness, and said mental health challenges are easier to address when people are housed. But respondents from the city of Fontana, California commented, “Hiding someone away in an apartment or hotel room does not cure them from mental illness. Housing first without mental health support DOES NOT WORK.” [SIC]
Officials from Issaquah, Washington, observed: “Stable housing must be coupled with other intensive support services. Housing alone does not improve mental health outcomes.” They added that for chronically unhoused people, “adjusting to living indoors is often underestimated and if housing is not accompanied by extra supports to help with the transition, people are more likely to fall back into homelessness.”
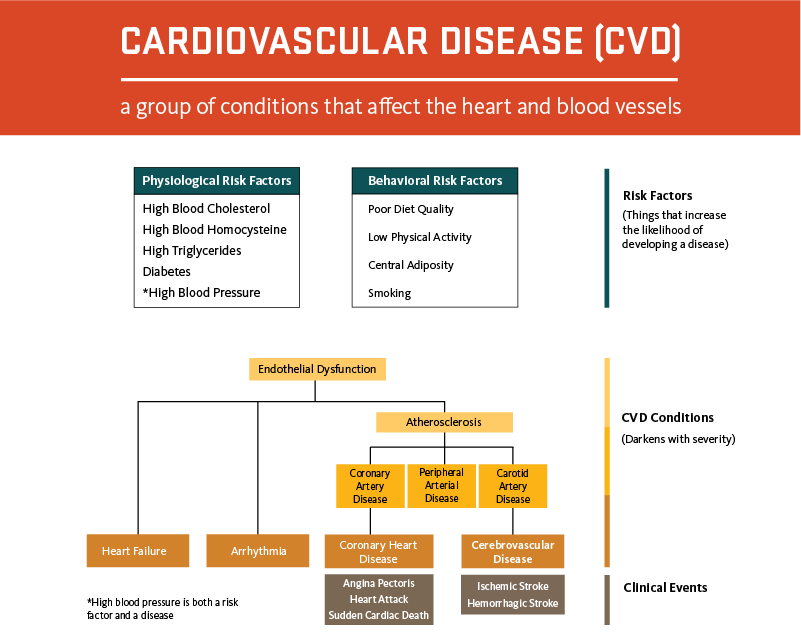
Cardiovascular Disease Is Primed to Kill More Older Adults, Especially Blacks and Hispanics
Cardiovascular disease — the No. 1 cause of death among people 65 and older — is poised to become more prevalent in the years ahead, disproportionately affecting Black and Hispanic communities and exacting an enormous toll on the health and quality of life of older Americans.
The estimates are sobering: By 2060, the prevalence of ischemic heart disease (a condition caused by blocked arteries and also known as coronary artery disease) is projected to rise 31% compared with 2025; heart failure will increase 33%; heart attacks will grow by 30%; and strokes will increase by 34%, according to a team of researchers from Harvard and other institutions. The greatest increase will come between 2025 and 2030, they predicted.
The dramatic expansion of the U.S. aging population (cardiovascular disease is far more common in older adults than in younger people) and rising numbers of people with conditions that put them at risk of heart disease and stroke — high blood pressure, diabetes, and obesity foremost among them — are expected to contribute to this alarming scenario.
Because the risk factors are more common among Black and Hispanic populations, cardiovascular illness and death will become even more common for these groups, the researchers predicted. (Hispanic people can be of any race or combination of races.)
“Disparities in the burden of cardiovascular disease are only going to be exacerbated” unless targeted efforts are made to strengthen health education, expand prevention, and improve access to effective therapies, wrote the authors of an accompanying editorial, from Stony Brook University in New York and Baylor University Medical Center in Texas.
“Whatever focus we’ve had before on managing [cardiovascular] disease risk in Black and Hispanic Americans, we need to redouble our efforts,” said Clyde Yancy, chief of cardiology and vice dean for diversity and inclusion at Northwestern University’s Feinberg School of Medicine in Chicago, who was not involved with the research.
Of course, medical advances, public health policies, and other developments could alter the outlook for cardiovascular disease over the next several decades.
More than 80% of cardiovascular deaths occur among adults 65 or older. For about a dozen years, the total number of cardiovascular deaths in this age group has steadily ticked upward, as the ranks of older adults have expanded and previous progress in curbing fatalities from heart disease and strokes has been undermined by Americans’ expanding waistlines, poor diets, and physical inactivity.
Among people 65 and older, cardiovascular deaths plunged 22% between 1999 and 2010, according to data from the National Heart, Lung, and Blood Institute — a testament to new medical and surgical therapies and treatments and a sharp decline in smoking, among other public health initiatives. Then between 2011 and 2019, deaths climbed 13%.
The covid-19 pandemic has also added to the death toll, with coronavirus infections causing serious complications such as blood clots and millions of seniors avoiding seeking medical care out of fear of becoming infected. Most affected have been low-income individuals, and older non-Hispanic Black and Hispanic people, who have died from the virus at disproportionately higher rates than non-Hispanic white people.
“The pandemic laid bare ongoing health inequities,” and that has fueled a new wave of research into disparities across various medical conditions and their causes, said Nakela Cook, a cardiologist and executive director of the Patient-Centered Outcomes Research Institute, an independent organization authorized by Congress.
One of the most detailed examinations yet, published in JAMA Cardiology in March, examined mortality rates in Hispanic, non-Hispanic Black, and non-Hispanic white populations from 1990 to 2019 in all 50 states and the District of Columbia. It showed that Black men remain at the highest risk of dying from cardiovascular disease, especially in Southern states along the Mississippi River and in the northern Midwest. (The age-adjusted mortality rate from cardiovascular disease for Black men in 2019 was 245 per 100,000, compared with 191 per 100,000 for white men and 135 per 100,000 for Hispanic men. Results for women within each demographic were lower.)
Progress stemming deaths from cardiovascular disease in Black men slowed considerably between 2010 and 2019. Across the country, cardiovascular deaths for that group dropped 13%, far less than the 28% decline from 2000 to 2010 and 19% decline from 1990 to 2000. In the regions where Black men were most at risk, the picture was even worse: In Mississippi, for instance, deaths of Black men fell only 1% from 2010 to 2019, while in Michigan they dropped 4%. In the District of Columbia, they actually rose, by nearly 5%.
While individual lifestyles are partly responsible for the unequal burden of cardiovascular disease, the American Heart Association’s 2017 scientific statement on the cardiovascular health of African Americans notes that “perceived racial discrimination” and related stress are associated with hypertension, obesity, persistent inflammation, and other clinical processes that raise the risk of cardiovascular disease.
Though Black people are deeply affected, so are other racial and ethnic minorities who experience adversity in their day-to-day lives, several experts noted. However, recent studies of cardiovascular deaths don’t feature some of these groups, including Asian Americans and Native Americans.
What are the implications for the future? Noting significant variations in cardiovascular health outcomes by geographic location, Alain Bertoni, an internist and professor of epidemiology and prevention at Wake Forest University School of Medicine, said, “We may need different solutions in different parts of the country.”
Gregory Roth, a co-author of the JAMA Cardiology paper and an associate professor of cardiology at the University of Washington School of Medicine, called for a renewed effort to educate people in at-risk communities about “modifiable risk factors” — high blood pressure, high cholesterol, obesity, diabetes, smoking, inadequate physical activity, unhealthy diet, and insufficient sleep. The American Heart Association has suggestions on its website for promoting cardiovascular health in each of these areas.
Michelle Albert, a cardiologist and the current president of the American Heart Association, said more attention needs to be paid in medical education to “social determinants of health” — including income, education, housing, neighborhood environments, and community characteristics — so the health care workforce is better prepared to address unmet health needs in vulnerable populations.
Natalie Bello, a cardiologist and the director of hypertension research at the Smidt Heart Institute at Cedars-Sinai Medical Center in Los Angeles, said, “We really need to be going into vulnerable communities and reaching people where they’re at to increase their knowledge of risk factors and how to reduce them.” This could mean deploying community health workers more broadly or expanding innovative programs like ones that bring pharmacists into Black-owned barbershops to educate Black men about high blood pressure, she suggested.
“Now, more than ever, we have the medical therapies and technologies in place to treat cardiovascular conditions,” said Rishi Wadhera, a cardiologist and section head of health policy and equity research at the Smith Center for Outcomes Research in Cardiology at Beth Israel Deaconess Medical Center in Boston. What’s needed, he said, are more vigorous efforts to ensure all older patients, including those from disadvantaged communities, are connected with primary care physicians and receive appropriate screening and treatment for cardiovascular risk factors, and high-quality, evidence-based care in the event of heart failure, a heart attack, or a stroke.